The Food Is Medicine Coalition and Partners Release a New Framework
References: fimcoalition.org
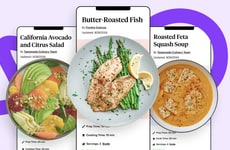
The Food Is Medicine Coalition, in collaboration with the Center for Health Law and Policy Innovation at Harvard Law School and with support from the Dohmen Company Foundation, has released the Medically Tailored Meal Sustainability Blueprint — a comprehensive national framework designed to guide the integration of medically tailored meals into the broader U.S. healthcare system.
The Medically Tailored Meal Sustainability Blueprint addresses the longstanding challenge of moving nutrition-based interventions from temporary, grant-funded pilot programs toward sustainable, reimbursable services covered by healthcare payers. The document outlines key considerations across legal, regulatory, and operational domains. It establishes consistent standards for eligibility, provider qualifications, service delivery, and program integrity.
The Food Is Medicine Coalition's ultimate goal is to create a predictable and high-quality foundation that can be adopted by policymakers, health systems, and community-based organizations nationwide.
Image Credit: Food Is Medicine Coalition x Harvard Law School
The Medically Tailored Meal Sustainability Blueprint addresses the longstanding challenge of moving nutrition-based interventions from temporary, grant-funded pilot programs toward sustainable, reimbursable services covered by healthcare payers. The document outlines key considerations across legal, regulatory, and operational domains. It establishes consistent standards for eligibility, provider qualifications, service delivery, and program integrity.
The Food Is Medicine Coalition's ultimate goal is to create a predictable and high-quality foundation that can be adopted by policymakers, health systems, and community-based organizations nationwide.
Image Credit: Food Is Medicine Coalition x Harvard Law School
Trend Themes
-
Medically Tailored Nutrition Reimbursement — Emerging reimbursement frameworks for medically tailored meals could upend traditional benefits by embedding nutrition as a billable clinical service within payer contracts.
-
Standardized Eligibility and Provider Qualifications — The push for consistent standards across eligibility and provider credentials may enable scalable credentialing platforms and verification services that shift how nutrition care is sourced and delivered.
-
Integration of Nutrition Into Clinical Pathways — Embedding nutrition protocols into care pathways has the potential to reconfigure care management workflows and redefine provider roles around food-as-treatment models.
Industry Implications
-
Health Insurance — Payer organizations face opportunities to redesign coverage models and risk-sharing arrangements around documented clinical outcomes tied to medically tailored meals.
-
Hospital and Health Systems — Health systems could see operational transformation as inpatient and post-discharge programs incorporate reimbursable meal services into care coordination and readmission reduction strategies.
-
Community-based Food Services — Local nonprofit and social enterprise food providers may evolve into certified clinical vendors, altering funding mixes and partnerships with medical institutions.
8.4
Score
Popularity
Activity
Freshness