Preparing Hospitals for COVID-19
We Spoke with Mark Graban to See How the US is Managing Surges (GALLERY)
Related Trend Reports
Branding, Business, Drinking, Health, Lifestyle, Marketing, Multimedia, New Ventures, Social Business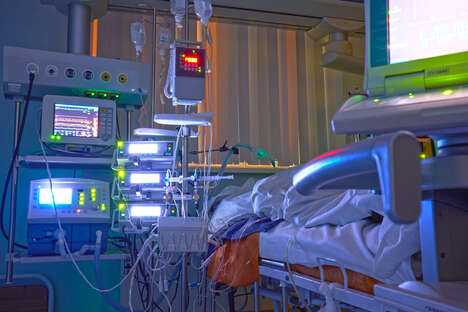



What are hospitals in the US doing to prepare for the increase in COVID-19 cases?
There are widespread preparation efforts, which include screening patients for respiratory symptoms before they enter an emergency room or a clinic. Hospitals need to keep possible COVID-19 patients away from patients who need other care. While it’s still a challenge, they are working to gain better access to testing, even if that means developing their own tests in some cases. Hospitals are also trying to free up as much intensive care (ICU) capacity as possible by postponing elective surgical procedures. The final challenge is making sure there are enough supplies, like masks, and that all staff are properly trained on COVID-19-related protocols. From news and social media reports, not every hospital is equally prepared, unfortunately, but this is improving hour-by-hour.
How will hospitals manage their current patient load, while preventing these patients from catching COVID-19?
The best practices include separating patients with respiratory systems, by having a separate waiting room, putting symptomatic patients in isolation rooms, or using more creative solutions like tents or specialized facilities that are dedicated to potential COVID-19 patients. It’s also critically important that patients only go to their doctor or an emergency room if they have shortness of breath and difficulty breathing. If you have just a fever and a cough, make a phone call to a doctor or an emergency room before arriving. They can triage you over the phone. It’s important to not clog up waiting rooms and you want to minimize the exposure to other people.
With an increase in demand for masks and personal protective equipment, how will hospitals ensure the safety of frontline staff if there are shortages?
The honest reality is that shortages and rationing of masks is being reported in news outlets and by healthcare providers on social media. Asking nurses to re-use masks all day is something that needs to stop. If the federal government has masks in a strategic supply, they need to be released now. Mask manufacturers need to ramp up production immediately. We need to do more to ensure the safety of patients and frontline staff. A shortage of masks or the improper use of masks puts people in harm’s way.
Is it possible for the US healthcare system to meet the surge in demand?
Experts have been saying for weeks that hospitals in the U.S. don’t have enough ICU beds or enough ventilators. The nurses and doctors that we have might also be stretched too thin if there’s a large enough spike in demand, especially if some of them become sick. That’s why it’s critically important for everybody to help “flatten the curve” by staying home as much as possible, also known as “social isolation” or “physical isolation.” The federal government also says they are releasing ventilators from a strategic national stockpile, and the military can provide assistance through Navy hospital ships or Army field hospitals that could be set up.
How has the delay in COVID-19 testing impacted the healthcare system’s readiness?
Having a test (or not having it), will not affect the care of specific individuals, as people with COVID-19 symptoms are being treated presumptively. That is what the healthcare system does whenever Influenza rates are high in a particular year, they treat them presumptively. The problem with not having enough tests is several-fold. For one, we don’t know how bad the problem is, so hospitals can’t prepare. Individuals also don’t know if they have the disease, so they don’t know if they need to quarantine. It is a major problem and is contributing to some people not taking the pandemic seriously, which also prevents others from knowing how much they need to prepare.
How can staff and visitors maintain their safety throughout the pandemic?
Hospitals are generally limiting visitors to one per patient. In general, if you have respiratory symptoms, you should stay home—which means not visiting the hospital or going with others. Hospitals are screening visitors and trying to keep those who are coughing or sneezing from entering. Some might do temperature checks, as well. Staff need to use personal protective equipment (PPE) properly and everybody should wash their hands with soap and water (for 20 seconds), or use hand sanitizer as often as possible. Again, isolating patients with respiratory symptoms and including strategies like drive-up testing, can help prevent the spread.
What is being done for those who don’t have access to health insurance, and can’t afford the out-of-pocket costs associated with treatment for the virus?
As part of the coronavirus relief package that was signed into law this week, there are provisions for free COVID-19 testing, although availability is still a problem. The law also provides workers with two weeks of paid sick leave if they are being tested, or if they have been diagnosed with COVID-19. That’s all that has been passed at this point. Paying for treatment is an unresolved issue, as one report says that even those with insurance might pay $1,300 or more out-of-pocket for COVID-19 treatment.
Do you believe the pandemic will result in permanent changes to the country’s healthcare system?
Hopefully, this will be a 9/11-style wake-up call that leads to greater preparedness and coordination in the future. ICU beds are very full in normal circumstances, but it’s hard to ask hospitals to invest in capacity that might only be needed in rare surges. People might expect the government and the military to be part of ongoing surge readiness, especially if medical ships and field hospitals prove helpful during this crisis, but hopefully they are not needed.
References: markgraban, kainexus
Featured Articles

CO2-Made Hand Sanitizers
The Air Co. Hand Sanitizer is Being Made by the Vodka Brand

Virtual Whiskey Events
The Virtual Whiskey Show Supports At-Home Sampling

Self-Isolation Dance Parties
'Stevie' is a New Short Dance Film Examining the Mind of a Teen

Gin-Based Hand Sanitizers
58 Gin Distillery Made an Alcohol Hand Sanitizer for the Benevolent Ball

Livestreamed Shark Tanks
Ripley's Aquarium of Canada Launched a Shark Camera to Enjoy in Isolation

Discounted Period Product Deliveries
Menstruation Product Company Rael Helps Women Amid COVID-19

Skincare Medical-Grade Disinfectants
Nivea-Maker Beiersdorf Changes Production to Fight COVID-19

Free Return Flights
Sunwing is Offering Free Return Flights to Stranded Passengers
Streamlined Group Call Updates
Microsoft Teams Added New Features to Improve Group Calls